For two weeks I tracked my blood glucose (aka “blood sugar”) levels with a Continuous Glucose Monitor (CGM). A CGM is a small device about the size of 2 stacked quarters that you apply to your arm. It has a very tiny needle and some strong adhesive that allows the device to stick for 14 days.
I’m not a big fan of needles, so this was a much better alternative to sticking my finger each time I wanted a reading.
Learning about blood glucose
Before starting the monitoring I took some time to educate myself on blood glucose in order to set some realistic goals. Here’s what I learned:
- Blood glucose is the primary energy source for all the cells in our body. Cells use insulin to process blood glucose and convert it into energy. In a typical diet, blood glucose levels rise after a meal, and then fall as the body processes the glucose.
- The body can very easily convert carbohydrates into sugar. Eating a lot of sugar, or a lot of carbs, can cause blood glucose levels to raise to high levels. Your body should naturally lower blood glucose levels by producing insulin.
- When blood glucose levels rise and fall quickly within a short period of time, this is called a “spike”. These spikes are not ideal for many reasons, but the most important to me at the moment is Pancreas Beta Cell Exhaustion. In layman’s terms I sort of understand, this basically means that the pancreas is “wearing out” (from overproducing insulin to deal with high blood glucose levels) and that I’m at risk of diabetes.
- The CDC guidance on managing blood glucose:
- Before a meal, in a fasted state, blood glucose levels should range between 80-130mg/dL.
- 2 hours after the start of a meal, in a fed state, blood glucose should measure less than 180mg/dL.
- The disclaimer for these numbers on their site: “Your blood sugar targets may be different depending on your age, any additional health problems you have, and other factors.”
The goals I set with all this in mind
- Target a daily blood glucose range 95-140mg/dL
- This isn’t the most optimal range, but without knowing what to expect, it seemed more realistic for the beginnings of a low carb diet.
- Minimize blood glucose spikes altogether with diet alone
- This would indicate that I’m remaining on target with my low carb diet along with intermittent fasting.
- Understand how my diet, intermittent fasting, and exercise impacts my blood glucose levels while on Metformin.
- I’ve removed the majority of carbs and sugar from my diet, so I expected spikes to be minimal.
- I didn’t know what to expect for my fasting blood glucose levels though.
- I’m still learning a lot about Metformin, so I’ll post my notes to cover this medication separately.
My blood glucose averages plotted for 14 days
Now that I’m finished monitoring with my first device, I wanted to share the results. They’re far better than I was expecting!
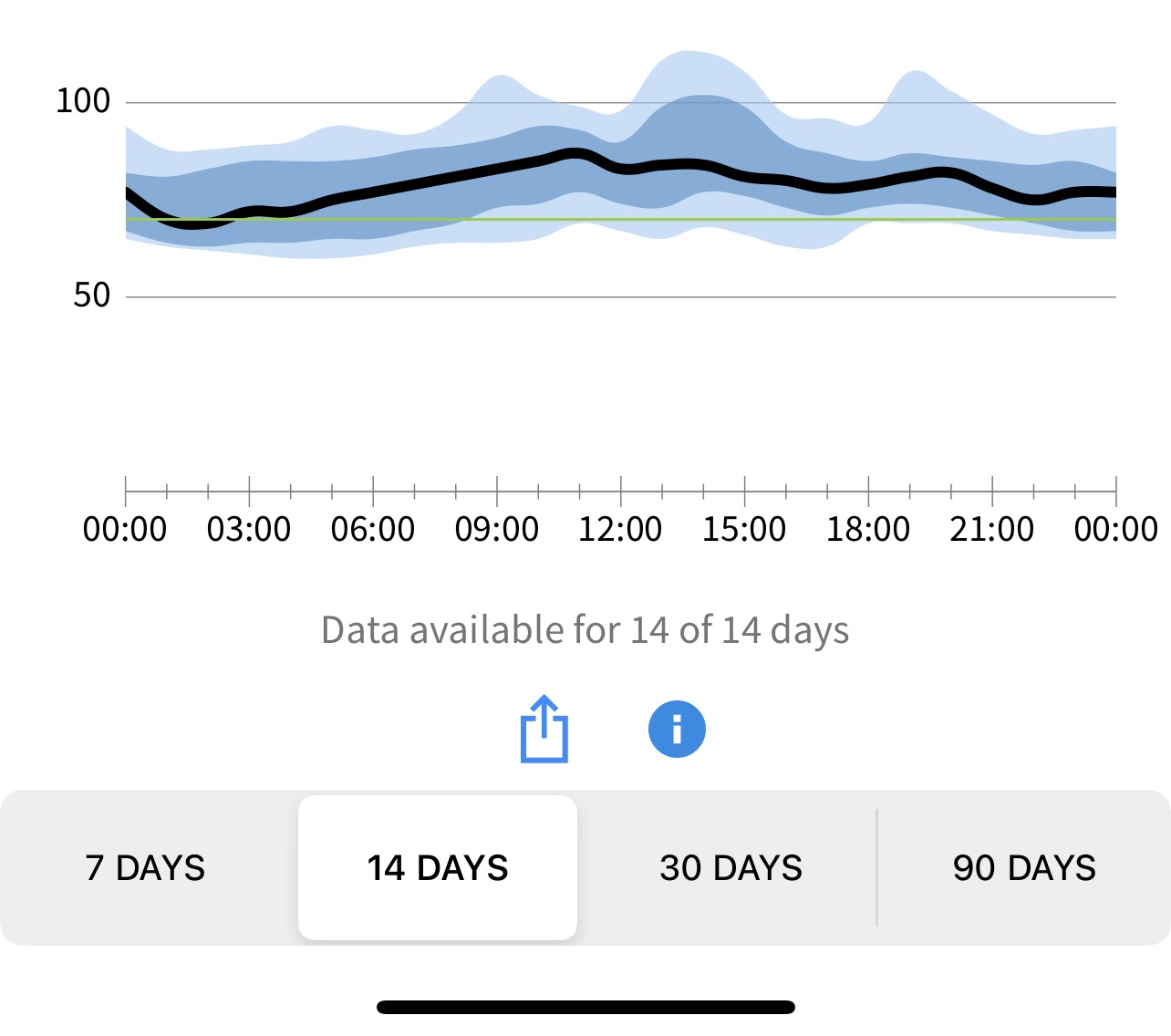
So what does this mean?
- I’m doing better than I was expecting! My diet and intermittent fasting has a lot to do with the awesome results I’m seeing today.
- My daily blood glucose range is 70-85mg/dL. This is much better than where I assumed I would start.
- I mostly ate between 11am and 7pm for these 14 days. This aligns with my 16:8 intermittent fasting schedule.
- Overnight I fasted for 16 hours and maintained an average around 70mg/dL. This is on the lower end, but I’m also entering ketosis during this period and so not feeling any adverse effects of hypoglycemia.
What have I learned?
- Managing blood glucose spikes with diet alone is more challenging than I expected. Eventually I will learn which foods cause spikes for me, but I’m not there today.
- Walking longer distances for exercise:
- raised my blood glucose slightly in the mornings
- walking after a meal neutralized anticipated post-meal spikes
- Some low-carb and low-sugar foods still impact blood glucose levels in unexpected ways. (like this sugar free gum)

It’s one thing to read about how all of this works, but it’s been a next-level experience witnessing all of this in my own body. I feel much more confident in my ability to manage my condition given what I’ve learned these past few weeks.
